What Is Endo Belly? A Complete Guide to Endometriosis Belly
If you live with endometriosis, you know the morning ritual: checking the mirror to see which “body” you’ve woken up with. Maybe at 8 AM, your stomach is flat. By 2 PM, you’re secretly unbuttoning your jeans under the table, your skin feels three sizes too small, and you’re sporting a belly that looks—quite literally—six months pregnant.
Or ... maybe you woke up with a belly already protruding over your pajamas.
Perhaps your "big belly" is often accompanied by some other symptoms of endo belly, like digestive distress that may include abdominal pain, severe stomach pain, cramps, diarrhea, constipation, nausea, oh my! We call it “Endo Belly,” but let’s be real: that term really simplifies a symptom that felt, for me, like a biological hurricane. It hits during your period, or it doesn’t. Severe swelling flares after an apple, or it happens when you haven’t eaten a thing. It’s rock-hard, painful, and deeply unpredictable; or maybe it's squishy and looks like you suddenly gained 10 pounds.
It's radical-- I mean, how could intense abdominal distension and gastrointestinal discomfort not significantly impact daily life-- yet, we're often still told to drink ginger tea or meditate.
Here is the truth: Endo belly isn’t "just gas,” and it isn't even always associated with endometriosis! It is a visible, vibrating reflection of your internal systems colliding—from “leaky” endotoxins and wonky pelvic mechanics to your nervous system screaming at your gut. Endometriosis lesions may (obviously) also be to blame--along with scar tissue, adhesions, cysts, and adenomyosis-- but not always. Many women have a professional, excision surgery in hopes their bloating "pops" as well, yet it remains.
If you can relate, yet are sick of going from site to site being told to drink ginger tea and use castor oil packs, this guide is your home base for finally connecting those dots. If you want to explore each cause in depth, I have linked my deep-dive posts throughout this article.
Understanding the Endo Belly Equation: Bloating and/or Swelling Plus Distention
First of all, endo belly refers to a constellation of symptoms. It is not a diagnosis. It is not one thing caused by one thing that all sufferers alike face. Also, it's not " just some bloating." Usually, it is more of an equation that is akin to this:
Endo Belly = a) swelling and/or b) bloating + c) distention
While we often use some of those terms interchangeably, clinical research makes a sharp distinction between them:
Bloating is a subjective, internal sensation of pressure, tightness, or "trapped gas." It can feel like pressure, yet there's no visible sign. You are filled with gas or food and feel the pressure!
Swelling is where endo gets unique. Unlike gas-based pressure increasing, swelling is an inflammatory event. It’s the result of your immune system flooding the pelvic or abdominal cavity with fluid (edema) and white blood cells in response to lesions, "leaky" endotoxins, bacteria, yeasts, or ruptured cysts. Swelling can build up like gas, increasing the amount of space taken up in the abdomen or pelvis.
Between bloating and swelling, that may mean you have a lot more "stuff" to fit in your abdomen and pelvis.
This is how one gets Distension: the objective, measurable increase in abdominal girth. Distension occurs when pressure builds inside the abdomen from multiple sources—gas, inflammation, fluid retention, muscular dysfunction, or organ displacement. In other words, the belly is not just bloated. It is physically expanding so much that it can no longer be "contained" appropriately.
In other words, you can feel bloated or even swollen without your stomach actually changing size, but distension is the physical expansion that makes your pants tight (or makes us look pregnant). For those with endometriosis, this distinction is vital because distension often signals a not just gas but also a "mechanical" failure—like the diaphragm pushing down and the abdominal wall relaxing (abdomino-phrenic dyssynergia)—rather than just having "too much gas."
It's really what we refer to when we're referring to ENDO BELLY BLOAT, where we protrude in front of our frame.
Endo Belly Feel: What Is Your Endo Belly Equation?
As I write about at length in my book, Heal Endo: Endometriosis is unique because it's multi-factorial. That means many factors contribute to creating and progressing endometriosis, yet they don't line up equally for each sufferer. You may have a terrible bacterial overgrowth, while another sufferer has excess estrogen up the wazoo.
The same can be said for endo belly! There are many possibilities why you might be bloated. Many more reasons why you may be swollen. And still more as to why you may be distended. And truly? Your own issues may not align even with your best endo-friend, who also has a similarly severe abdominal bloating!
This is where my series on endo belly will help YOU. By looking at clues to understand why you're so bloated, swollen, or distended (I keep repeating this so you remember there are 3 main categories to investigate), you can identify the reasons for your digestive discomfort and start to deflate.
The exact cause of endo belly depends on YOU, dear reader, and may involve several overlapping mechanisms, including inflammation, tissue growth, body mechanics, hormonal influences, and more.
Below is a comprehensive list of answers for you to look through!
Part 1: Bloating
Bloating is the expansion of the contents of your digestive tract, and there are many reasons why yours would be expanding. Here are some clues
1. SIBO and IMO
Did you know that up to 92% of endo patients have SIBO (Small Intestinal Bacterial Overgrowth) or IMO (Intestinal Methanogen Overgrowth)? SIBO can also cause digestive issues like GERD, chronic constipation, or diarrhea, and is known for its extreme ability to bloat and distend any belly that has it. It's also a leading root cause for irritable bowel syndrome, and it may be a root driver for some of your worst endo symptoms as well. With nearly all of us (potentially) suffering from it, addressing SIBO or IMO becomes one of the main tenets to pop any endo belly out there.
The Connection: Understand the link between Endo, IBS, and SIBO.
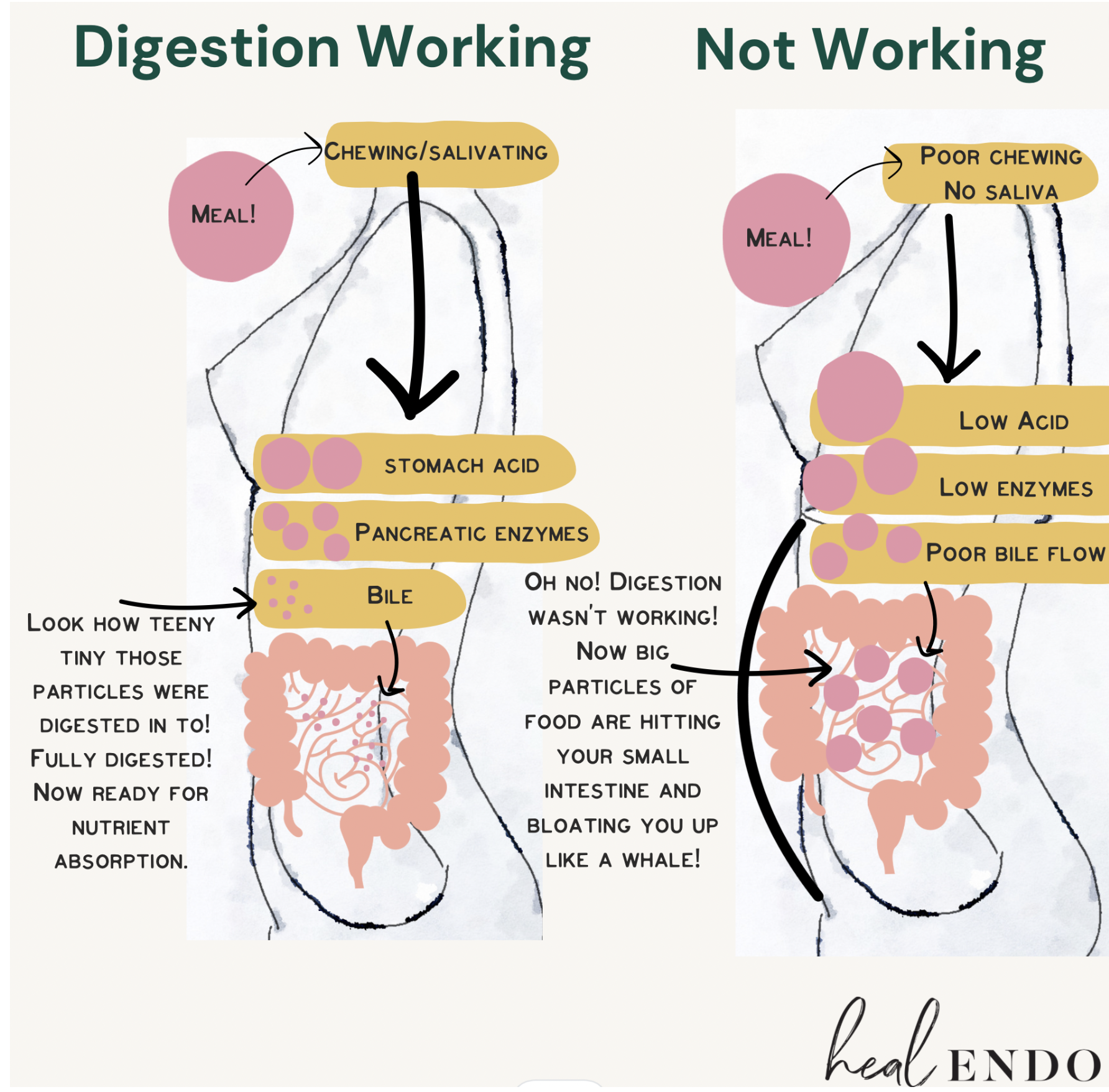
2. Poor Digestion
Did you know that "endo belly" is often a result of simple digestive insufficiency? This happens when your body fails to properly break down food into microscopic particles, leaving "undigested chunks" to travel through your system. These fragments don’t just sit there; they ferment and putrefy in your 98-degree digestive tract, creating gas that acts like a "blown lid" on a blender, causing extreme pressure and abdominal distension. For many endo warriors, the belly isn't just reacting to the disease—it’s reacting to the "bricks" of food it can't process.
The Connection: Learn how chewing, stomach acid, and meal spacing act as the first line of defense against the fermentation that causes endo belly.
Part 2: Swelling
1. Dysbiosis and Endotoxins (The Inflammation Trigger)
This is the “endo-elephant” in the room. Nearly all of us with endo have an imbalance of bacteria in our gut. When “bad” (gram-negative) bacteria die or grow, they release endotoxins (LPS). If you have a leaky gut, these endotoxins slip into your bloodstream and pelvic cavity, triggering an all-out immune war. This immune response can cause swelling and gastrointestinal symptoms, such as bloating, pain, and discomfort.
Deep Dive:Read more about how endotoxins and dysbiosis drive endo belly.
2. Reproductive Tract Dysbiosis (The Pelvic Leak)
We often talk about the gut, but your reproductive tract has its own microbiome, too. When “bad” bacterial strains of E. coli or Streptococcus proliferate in the uterus or cervix, they can travel through the fallopian tubes and into the pelvic cavity (thanks to retrograde menstruation). This dumps millions of endotoxins directly onto your pelvic organs, fueling the fire of endo lesions and causing localized swelling that radiates outward
The Problem:Is your reproductive tract microbiome fueling your endo belly?
3. The Iliocecal Valve “Hot Spot” (Localized Tissue Inflammation)
Sometimes endo belly isn’t a whole-abdomen event; it starts in one specific, angry corner: The ileocecal valve. When food particles get trapped here, it can become a breeding ground for bacteria and stagnation, leading to inflammation and potentially being a leading cause for SIBO.
The Map: How to identify and soothe your Endo Belly Hot Spot.
4. Endometriosis, Cysts, and Pelvic Inflammation
Endometriosis is an inflammatory condition in which tissue similar to the uterine lining, known as endometrial-like tissue, grows outside the uterus. This endometrial-like tissue releases inflammatory mediators, including prostaglandins and cytokines, which (along with trapped blood) can irritate surrounding tissue and contribute to swelling and discomfort in the abdomen and pelvis. The inflammatory response caused by this tissue can also irritate the intestines and other organs, particularly around the time of your period.
Obviously, this could cause some swelling!
The Book:If you want to learn all about endometriosis, you must read my book
5. Hormonal and Metabolic Changes
Did you know that your hormones act like a thermostat for your body’s fluid balance? In endometriosis, Estrogen Dominance can be a major driver of "endo belly." Estrogen is a "pro-growth" hormone that signals your body to retain salt and water. When estrogen is high (especially right before your period), it causes your pelvic tissues and intestinal walls to soak up fluid like a sponge. This isn't gas that you can "get rid of"; it is actual cellular swelling that makes your entire midsection feel heavy, tight, and "thick" to the touch.
The Connection coming soon: Understand how High Estrogen and Insulin resistance signal your kidneys to hang onto sodium, leading to systemic water retention.
Part 3: Distention
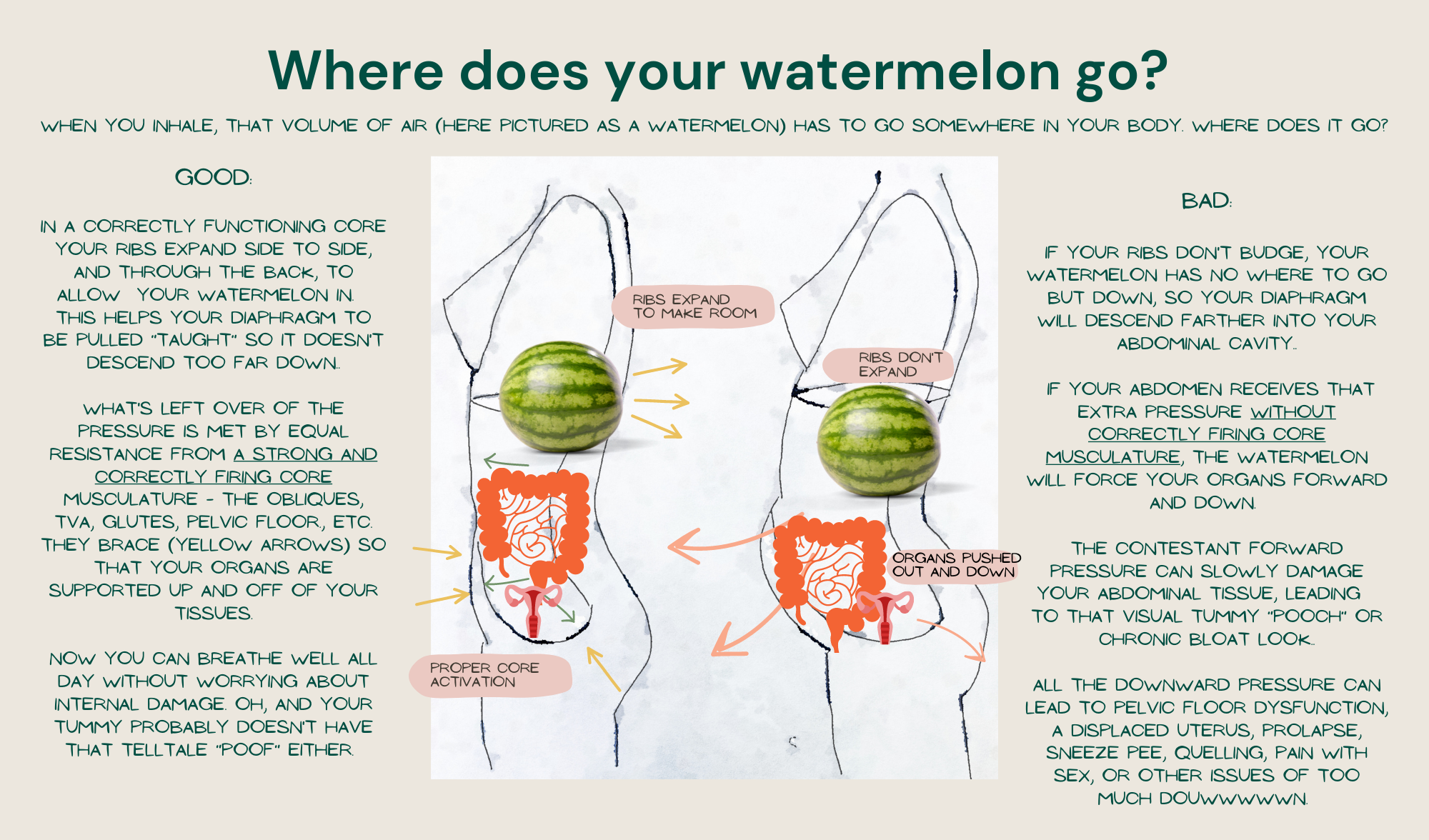
1. Core Dysfunction and the "Lower Belly Pooch"
Distention is often just as about how your muscles are holding you as it is what's pushing out (like gas or swelling). That's because 50% of people who are bloated don't look it! The other half? They may have muscular and diaphragm dysfunction that prevents the proper "holding up" of the organs. In addition, chronic pelvic pain, bloating, and/or inflammation causes us to “brace” our abdominals, which can lead to a weakened core and a lower-belly pooch that won’t go away, even when the inflammation subsides.
The Fix: How core dysfunction contributes to abdominal bloating.
2. Posture and Severe Bloating
Did you know that how you stand can determine how much your belly sticks out? When you live with chronic pelvic pain, your body naturally adopts a "protective" posture. You might tuck your tailbone under or arch your back excessively to move away from the pain. This shift in alignment weakens the Deep Core (the Transverse Abdominis) and the Pelvic Floor. Without these muscles acting as a "natural corset" to hold your internal organs in place, your intestines literally migrate forward and down. This results in a "pooch" or distension that isn't caused by gas at all, but by a lack of structural support.
3. The Anatomical Wildcard: Redundant Colons
This is the piece of the puzzle most doctors miss. Some of us are born with an extra-long colon (redundant colon). When you add endo-related inflammation to a colon that already has “too many loops,” you get a recipe for chronic constipation and extreme distension. Anatomical variations like a redundant colon can also lead to irregular bowel movements and sometimes painful bowel movements, especially during endo flare-ups. While this isn't wildly common, reseach shows that 30% of women with bowel endometriosis may have one (I know I do!).
The Secret:The endo belly problem you’ve never heard of: A redundant colon.
4. Adenomyosis and/or Adhesions
When you have Adenomyosis, the uterine wall thickens and the entire organ becomes "globular" and enlarged—sometimes reaching the size of a 12-to-15 week pregnancy. This occupies a massive amount of real estate in your pelvis, pushing your other organs upward and outward. When combined with Adhesions (bands of scar tissue that act like internal superglue), your intestines can become "tethered," or stuck to your abdominal wall. When your gut tries to move food or expand naturally, it hits these physical "straps," causing the belly to swell and protrude as it struggles against the restriction.
The Connection coming soon: Understand how physical crowding and organ "tethering" create a permanent or cyclical "pooch" that no amount of dieting can fix.
Diagnosing Your Own Endo Belly
In order to understand the reasons behind your own a) bloating, b) swelling, and c) distension, we need to investigate clues! To do so, we can begin looking at patterns:
• timing of symptoms around the menstrual cycle: are they cyclical in nature or constant
• relationship to meals and foods: is there a FODMAP link, dairy, wheat, or stress?
• associated digestive symptoms: do you just have bloating, or also nausea, or diarhea, or something else?
• imaging or surgical findings of endometriosis: do you know there are mechanical issues at play?
• results of a pelvic exam, which can help assess for cysts, scars, or other issues
Tracking symptoms over time can be extremely helpful in identifying patterns. Keeping a food diary can help you identify patterns that may suggest what makes your endo belly symptoms worse.
Managing Endo Belly
Because endo belly has multiple causes, management often requires addressing several systems at once. To effectively manage endometriosis-related swelling and ease bloating, it’s important to use a combination of strategies tailored to your needs.
Diet and lifestyle treatment options
Of course, I'm a huge fan of anti inflammatory diet and lifestyle changes that can help reduce the look of a bloated belly pretty fast in many of us, not to mention reduce endometriosis symptoms. Even just trying a lowFODMAP diet for 2-4 weeks, while increasing hydration, can offer us a huge clue if there are (most likely) bacterial overgrowths like SIBO contributing to the painful bloating, irritable bowel syndrome ibs symptoms, and even contributing to painful periods.
It's important to identify foods that may trigger your symptoms, such as gluten, dairy, and processed sugars, as limiting them can often help reduce bloating and discomfort. Even normal, healthy foods can be inflammatory foods if your own body is reacting to them, which is why a short term elimination diet can be a helpful consideration. Many women find that dietary changes can fight inflammation within the digestive system. The best thing to do is keep a food diary, which can help you identify patterns and pinpoint which foods worsen your symptoms.
Managing stress is also important, as it can heighten gut sensitivity and worsen bloating.
If 92% of us have SIBO or IMO, 92% of us need to treat that
What we know is that 92% of all endo patients (not just the ones with gastrointestinal symptoms) may have SIBO and/or IMO. Because of the relation to immune dysfunction, endotoxemia, inflammation, and endometriosis, it's essential we address it! Like, really essential.
Pelvic floor and movement therapies
Core dysfunction and pelvic floor dysfunction can both contribute radically to that big, bloated look and heavy pelvic feel. This is why many of us (although I argue all of us) will benefit from pelvic floor physiotherapy, which can help restore coordination between the diaphragm, abdominal muscles, and pelvic floor.
Gentle breathing exercises and mobility work may also help reduce abdominal pressure. When lying down, incorporating deep belly breathing can help decrease tension in the lower abdominal region and relax the pelvic floor muscles, calm the nervous system, and reduce stress, which may decrease bloating and pain associated with endo belly.
Medical and surgical options
Truth be told, managing endometriosis itself through excision surgery can significantly reduce endo belly if the inflammation/swelling is indeed the underlying cause of your bloated abdomen and pelvis OR if the inflammation (or adhesions) are altering gut motility and contributing to other gastrointestinal symptoms. Scar tissue or adhesions may be making your own SIBO a recurring case that keeps coming back no matter how many times you treat it. In this case, to effectively alleviate endometriosis and endo belly, it is important to treat endometriosis directly through surgery. I recommend seeking out an endometriosis specialist directly to chat about your case (www.icarebetter.com is a great place to start).
Practical Tips To Prevent Endo Belly Flares
When distension is severe, simple measures can help reduce discomfort:
• If you have constipation, big bloating, and endo belly, Atantril is an incredible tool to consider! The therapeutic dose for severe cases is starting with 2 capsules, 3x a day, for one month. For me, with IMO and a redundant colon, Atantril has been a lifesaver.
• Avoid high FODMAP foods for a minute: the lowFODMAP diet may be a life saver for you while you get to the bottom of your severe bloating. I know almost for a fact that, if you have SIBO or IMO, a high FODMAP diet (which is actually really healthy), will worsen symptoms.
• If you have painful abdominal bloating, heat pads to relax muscle tissue can help
• Try gentle exercises like walking or yoga to help ease bloating and discomfort. Sometimes we need some aid with peristalsis (the moving of the intestinal tract), and gentle movement is the key here.
• Practice nervous system soothing techniques, such as mindfulness or visualization, to tap back into parasympathetic dominance. This is when your body prioritizes digestion (which is key!), and can over time shift your symptoms of endo belly--for some of us dramatically.
• Avoid activities that can worsen pain or core dysfunction, such as high-impact exercise, excess alcohol or sugar, blood sugar dysregulation, poor sleep, and unmanaged stress.
These approaches do not solve the root cause, but they can make flare-ups more manageable.
Endo Belly FAQs
Why do I look pregnant?
Severe abdominal distension from gas, inflammation, or muscle dysfunction can temporarily expand the abdomen.
Is endo belly just weight gain?
No. Endo belly is typically fluctuating distension, not fat accumulation.
Will hysterectomy stop endo belly?
Not necessarily. If digestive or biomechanical factors are involved, symptoms may persist!
Will addressing endo belly help with period pain?
It may reduce it, absolutely. That's because many of the same drivers of endo belly drive endometriosis symptoms (as I talk about at length in my book, there is a HUGE link with endometriosis and bacteria and the gut). So soothing the inflammation, balancing the gut and reproductive tract microbiome, and restoring core function could have a tremendous impact not just on your bowel habits and endo belly symptoms, but also on your endometriosis pain.
The Bigger Picture
Endo belly is not simply cosmetic bloating. It is a complex symptom that reflects interactions between inflammation, digestion, gut bacteria, muscle coordination, and pelvic anatomy.
Understanding those layers is the first step toward reclaiming your life! Believe me, I was there, in endo belly misery for decades.