Endo Belly Series Part 2: Core Dysfunction, Lower Belly Pooch, and Abdominal Bloating
When I had shi*ty, active endo and I found out there was a word for the shi*ty, enormous bloating associated with it—known as endo belly—I was enamored. “Endo Belly! Yes! There is a reason for my golum-like appearance!” I shouted to no one in particular. Not only did I have it, but other endo-folk also did. There’s oddly something comforting about knowing others out there had balloon-like bellies just like mine…
Not that it's great for anyone to have it; endo belly is a severe form of bloating experienced by individuals with endometriosis, often causing significant distress and impacting quality of life.
The problem was, I thought it was just another endometriosis symptom I couldn’t do much about. I couldn’t afford a properly done surgery at the time, and since I thought endo belly was “caused by endo,” there wasn’t much I could do, right? *Queue me spending $300 on Spanx products, not even kidding.
What little novice “me” didn’t understand is that endo belly is NOT a diagnosis. It’s simply a slang term referring to the significant bloating and digestive distress often experienced by those with endometriosis, and it may or may not be caused or provoked by the endo lesions themselves (as I’ll talk about below).
The most common symptom of endo belly is severe abdominal bloating, particularly just before or during your period. Endo belly refers to a specific symptom of endometriosis involving severe bloating and abdominal swelling that can mimic the appearance of pregnancy. Mine did, that’s for sure. The swelling from endo belly can fluctuate throughout the day and may worsen during certain phases of the menstrual cycle. Many people also experience related gastrointestinal issues such as constipation, diarrhea, or nausea.
Truly, it can be awful.
This is why I’m writing this series. To help you, dear reader, better understand the many reasons behind common symptoms of endo belly, like severe bloating, discomfort, and a feeling of pressure in the abdomen, perhaps even more during menstruation (but not necessarily). Mine was all the time!
THE ENDO BELLY SERIES
Now, I love really delving into the complex realities of endo-belly, and today we’re going to talk about one connection of many: the endometriosis-core dysfunction connection. I actually believe that, if you have endo-belly, no matter what driving force(s) are behind it you probably also have core dysfunction alongside.
Because the truth is, endo belly can be caused by many different things! Key causes of endo belly include inflammation, scar tissue, bowel sensitivity, and gut dysbiosis. The digestive system is often affected by endometriosis, leading to symptoms like bloating, discomfort, and slowed digestion. It’s also why I wrote this series for you! We will uncover the 5 big (like, endo belly big) factors that may be behind many of our endo bellies. Your endo belly may be provoked by one, two, three, four, or, well, all of them :) Check out any of these links for more info:
Lesions, Inflammation, and endo belly
For today, let’s chat core dysfunction, a big culprit for that lower belly pooch.
WHAT IS CORE DYSFUNCTION?
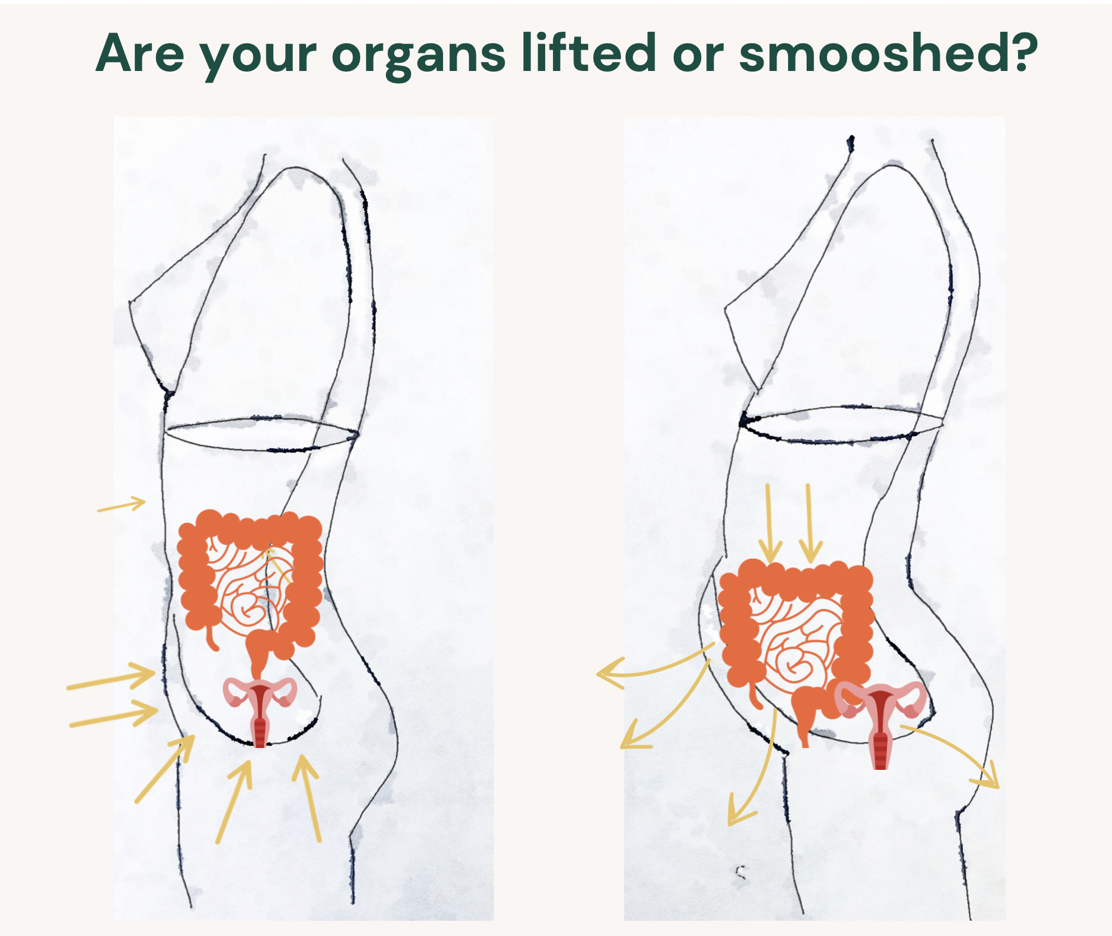
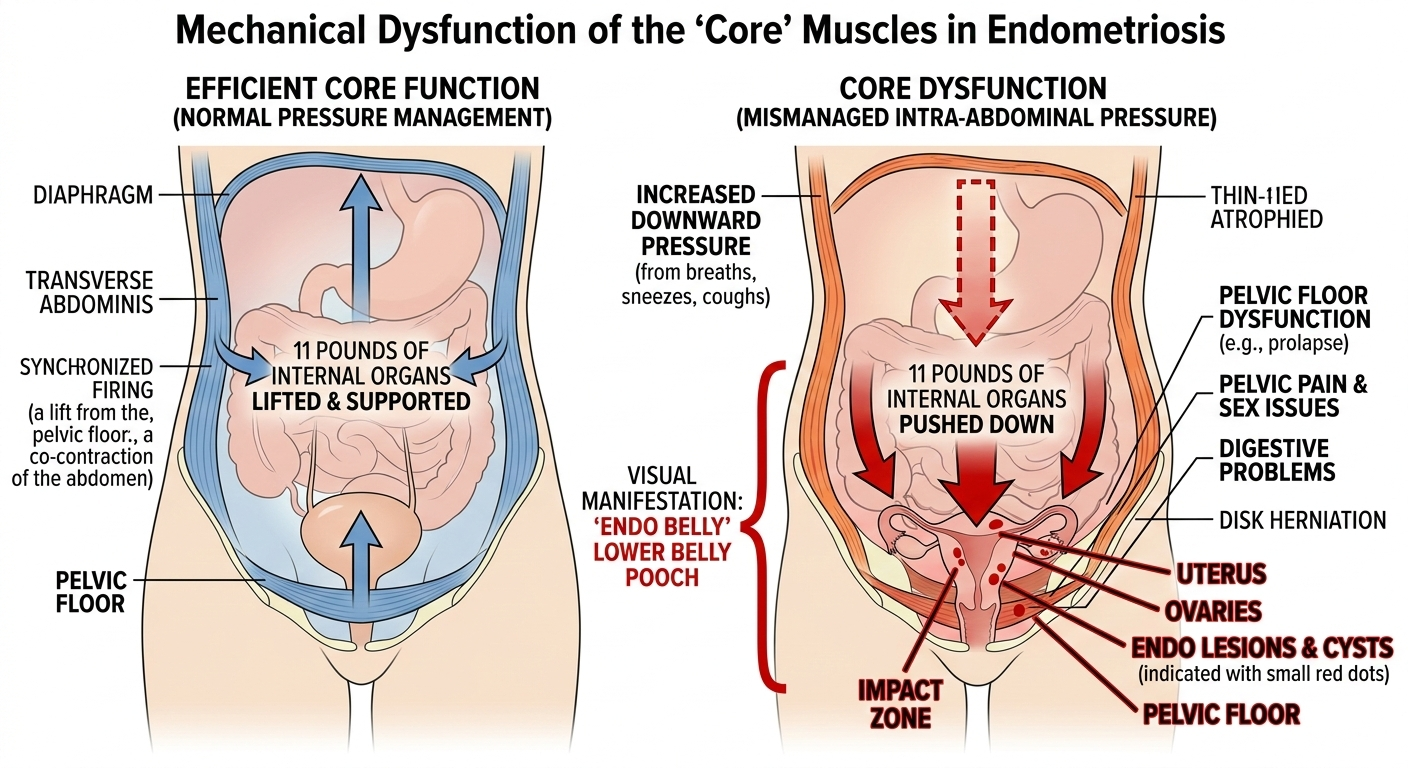
Core dysfunction specifically refers to the deep core musculature not firing properly when they should. Yet, I am not referring to what people usually think when they hear core (the six-pack muscles). Rather, I’m referring to the deep core muscles, which include the transverse abdominus, diaphragm, pelvic floor, and multifidus. Think of them as the muscles that encase your delicate organs, keeping them up and lifted (what we want), and intra-abdominal pressure low.
When your core is healthy and “married” to your movement, it performs a beautiful, synchronized dance behind the scenes. A functional core:
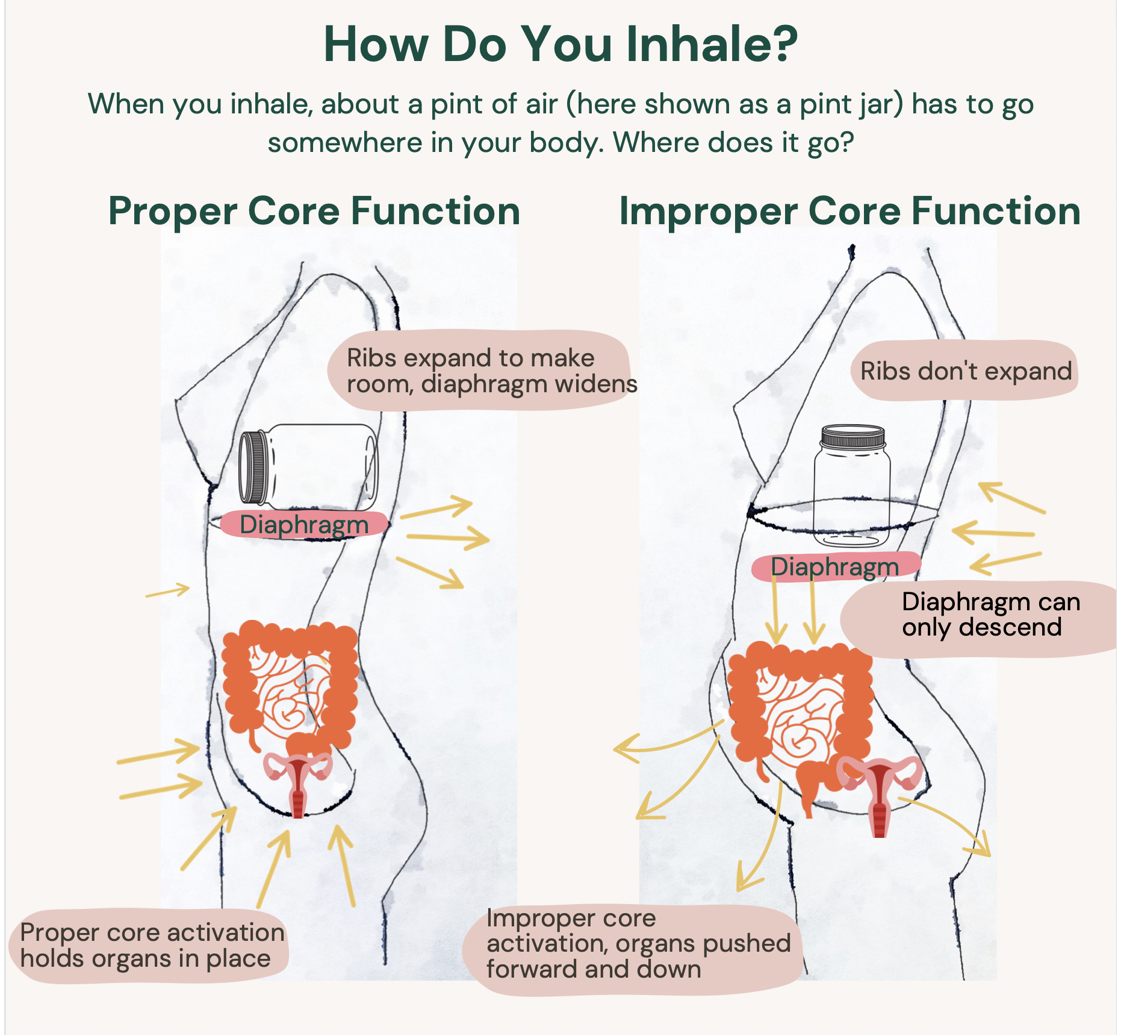
Allows for “Rib-First” Breathing: It lets your ribs expand wide and relaxed with every breath, rather than forcing your lower belly to balloon out to make room.
The “Smart-Brace” Reflex: It knows exactly when to kick into gear. Whether you’re lifting a heavy grocery bag or hit with a surprise “mega-sneeze,” your core should automatically brace to protect your spine and keep your “insides” from heading south.
The Power of Pro-Level Relaxation: A healthy core isn’t just “on” all the time. It knows how to actually relax. Constant tension isn’t strength—it’s just a recipe for exhaustion and a hard-to-the-touch belly.
The Pelvic Floor “Elevator”: Your core should be an expert at the “Lift and Let Go.” It needs to slightly activate and lift your pelvic floor up during a bracing move (like a run or a laugh), but it must be able to fully “drop the floor” and relax when you are farting, peeing, pooping, or having sex.
If your pelvic floor is stuck in a permanent “basement-on-fire” spasm because of endo pain, your ribs locked from permanent shallow breathing, and your transverse abdominus and multifundus so atrophied you can barely activate them … then it can’t do that lift-and-drop dance. It’s just stuck, confused, and eventually, it just stops answering the phone. This is core dysfunction.
When these muscles become dysfunctional, the organs are no longer up and lifted. Instead, they often become “pushed” downward (onto the pelvic floor, uterus, and delicate lady parts) and outward (resulting in that lower belly pooch or extreme looking bloating).
This look is often described as a “bloated belly”, especially in the context of endo belly, where the abdominal distension can be quite pronounced. Hormonal and metabolic changes, often triggered by stress, sleep deprivation, or diet, can further exacerbate abdominal distension in people with endometriosis. Additionally, fluid retention due to inflammation can contribute to the appearance of a bloated belly. Changes in gut bacteria and the presence of food intolerances may also play a role in digestive discomfort and bloating in endometriosis. However, just having this lower belly pooch does not automatically mean bloat (fluid or gas filling the space). The little belly pooch is often more of a visual of a biomechanical issue: your organs don’t have their “corset” on (i.e., deep core).
Add in gastrointestinal symptoms
Yet, when you then add in bloating (via hormones, gas, dysbiosis, SIBO, etc), those with endo belly now can report feeling like they look pregnant due to the severe level of bloating. During endo belly episodes, the abdomen can even feel hard or tight to the touch! Many people with endometriosis also experience painful bowel movements, especially during menstruation, as well as period pain. Trapped blood, enlarging cysts, and inflammation can contribute swelling. Additionally, endometriosis can lead to the formation of scar tissue, which may cause adhesions that affect the intestines and contribute to bloating and perhaps even more core dysfunction. Sigh.
This is why addressing core dysfunction becomes a vital part of any endo-belly healing protocol.
Core dysfunction increases INTRA-ABDOMINAL PRESSURE…AND that LOWER BELLY POOCH
I just mentioned something you may never have heard of: intra-abdominal pressure. “Pressure inside of me??” You gasp. Don’t worry, not pressure like a soda can (you don’t pop if someone pokes you). Intra-abdominal pressure refers to the slight pressure in your abdomen that increases as space decreases.
Like, if you take a huge breath (say a balloon’s worth of air in your lungs), that would increase the pressure in your abdomen. To accommodate, your deep core does a few things without squishing your organs into your pelvic floor and nether regions. Namely, your rib cage opens wide to make more room up north, while your pelvic floor and transverse abdominus brace a bit (holding you up and in down South) until you exhale.
This is how, when pressure increases (like inhaling air, or being super gassy), your deep core works together so your organs don’t fall out. Severe swelling and fluid retention from endometriosis can further increase intra-abdominal pressure, making the sensation much more intense than typical bloating. Severe distension during endo belly can also make clothing feel significantly tighter.
However, maybe your ribs are locked shut (like, do your ribs flow opwn when you take a breath?) and your deep core muscles are weak and your pelvic floor stuck in a spasm. Now you can’t manage the pressure correctly (core dysfunction), so the pressure-o-meter can go up too high, putting too much pressure on parts that don’t need it. Examples you can relate to:
Peeing your pants a little bit when you sneeze, laugh too hard, or jump on a trampoline. This is downward pressure
The “tampon slide,” when you’re walking or laughing or whatever and your tampon is pushed downnnnnn. More downward pressure
Feeling like you need to suck in 24/7 to look and feel supported. More outward pressure.
Doing never ending crunches and planks, and seeing your lower belly bulge growing (these are terrible for those with core dysfunction, is why)
Feeling a heavy pelvic pressure by 4 pm, and needing to put your legs up.
Seeing your tummy “loaf” when you do leg lifts or crunches rather than staying relatively flat (this is outward pressure)
HOW DOES CORE DYSFUNCTION DEVELOP FOR THE AVERAGE JO
Core dysfunction isn't some exclusive club only for those with endo—though we definitely seem to have VIP memberships. The truth is, most of us in the West are living lives that our deep core muscles find incredibly insulting.
We simply aren't using these muscles enough, or in the ways nature intended. This leads to atrophied (translation: very, very weak) deep core muscles that become stiff, inflexible, and altogether unable to "fire" together as a team.
Think about it: if you grew up fetching giant buckets of water from a nearby well every morning, your body would have learned—by sheer necessity—how to BRACE properly. You’d have to manage that internal pressure perfectly just to keep from toppling over or throwing out your back before breakfast. Your core would be "married" to your movement.
Fast forward to our modern reality. We are spectacularly sedentary. We sit in chairs for about 90% of our lives—office chairs, car seats, dining chairs, the "big comfy couch."
Chairs are basically core-killers. They don't ask your deep musculature to do anything. If we were all sitting cross-legged on the floor like our ancestors, our cores would be constantly, subtly "on" just to keep us upright. Instead, we lean back, let the furniture do the work, and our core effectively clocks out for the day.
When the core is turned off for most of our hours (and most of our years), we can’t exactly act surprised when it’s a bit dysfunctional, right? It’s like a sports team that hasn't practiced together in a decade—the second you ask them to handle a "high-pressure" event like a heavy sneeze or a HIIT workout, chaos ensues.
In addition, for aesthetic reasons, we’re often telling our core what to do rather than letting it work as it should. We suck in our flab, flex our abs, hold in farts, hold Kegels, and stand with poor posture to look more supermodel-eske.
CORE DYSFUNCTION ENSUES WITH ENDO AS WELL
It’s one thing to have a weak core because you sit in an office chair; it’s an entirely different beast when your core is literally guarding itself against a perceived internal attack. In endometriosis, endometrial tissue grows outside the uterus, causing inflammation that contributes to core and pelvic floor dysfunction. If you have endo, your core musculature isn’t just “out of shape”—it’s traumatized. Managing endometriosis as the underlying cause is essential for addressing core dysfunction and related symptoms, often requiring a multidisciplinary approach. Here is how the disease creates a specialized brand of core and pelvic floor dysfunction:
1. THE "GUARDING" REFLEX (THE PERMANENT CRUNCH)
Think about what happens when someone pretends they’re going to punch you in the stomach. You flinch, you round your shoulders, and you brace your abdominal wall.
Now, imagine having that “punch” coming from the inside 24/7 in the form of endometriosis lesions and chronic inflammation. Adopting strategies to fight inflammation, such as following an anti-inflammatory diet or reducing stress, can help manage these symptoms. Your brain eventually decides that the only way to protect your vital organs is to stay in a state of “perpetual bracing.” You are essentially doing a mini-crunch all day long just to handle the pain. This isn’t “strength”—it’s hypertonicity. Your muscles become so tight and “locked” that they lose the ability to actually moveand manage pressure.
Stress can worsen the symptoms of endometriosis, so reducing stress levels can help reduce endo belly symptoms.
2. PELVIC FLOOR DYSFUNCTION: THE BASEMENT IS ON FIRE
The pelvic floor is the literal floor of your core. When you have endo lesions o c a o if sitting on your broad ligament, your bladder, or your bowel, the surrounding muscles do what any muscle does when it's irritated: they spasm.
Over time, these muscles forget how to relax. This is why so many of us deal with painful sex, the "tampon slide," or the feeling that we can't fully empty our bladders. When the basement (your pelvic floor) is locked in a tight, upward spasm, it can't "catch" the pressure from your diaphragm. The result? That pressure has nowhere to go but out, pushing your lower belly into that unmistakable "pooch".
3. INFLAMMATION AS A "SPACE-TAKER"
Remember our airtight container? Chronic inflammation isn’t just a feeling; it involves actual fluid and swelling within the peritoneal cavity. This takes up physical space. Fluid retention due to inflammation is a key factor in the development of endo belly, as the body responds to irritation by holding onto excess fluid in the abdominal area.
When your insides are swollen, the “pressure-o-meter” is already in the yellow zone before you even take a breath. Your core muscles—already weak from the “Western chair life”—simply can’t keep up with the extra internal volume. They “give out,” and suddenly your organs are tipping forward and down.
Certain herbs and teas, such as turmeric and chamomile, are known for their anti-inflammatory properties and may help alleviate symptoms associated with endo belly.
4. THE CONFUSION CYCLE
Now your core isn't just weak; it's confused. It’s trying to "guard" against pain (tightness) while being unable to "brace" against movement (weakness). It’s like trying to drive a car with one foot on the brake and the other on the gas.
This is why "just doing more crunches" or planks, or leg lifts, usually makes core dysfunction worse! You're adding more "brake" to a system that is already locking up. To fix it, we have to teach the muscles that it's safe to let go, relax the ribs, and let the pressure distribute where it belongs.
HOW DO I KNOW IF I HAVE CORE DYSFUNCTION?
To differentiate between the many factors that cause bloating, watch symptoms! Note changes in bowel habits, bloating patterns, food triggers, etc, all important clues in differentiating endo belly from digestive or intestinal based bloating.
Keeping a food diary can help identify foods that ease or worsen endo belly symptoms and may reveal food intolerances or digestive issues. Nutrition counseling can also help identify foods that ease or worsen endo belly symptoms.
Also, here are a few tests you can do at home, right now to see if core dysfunction may be playing a major factor in your endo belly:
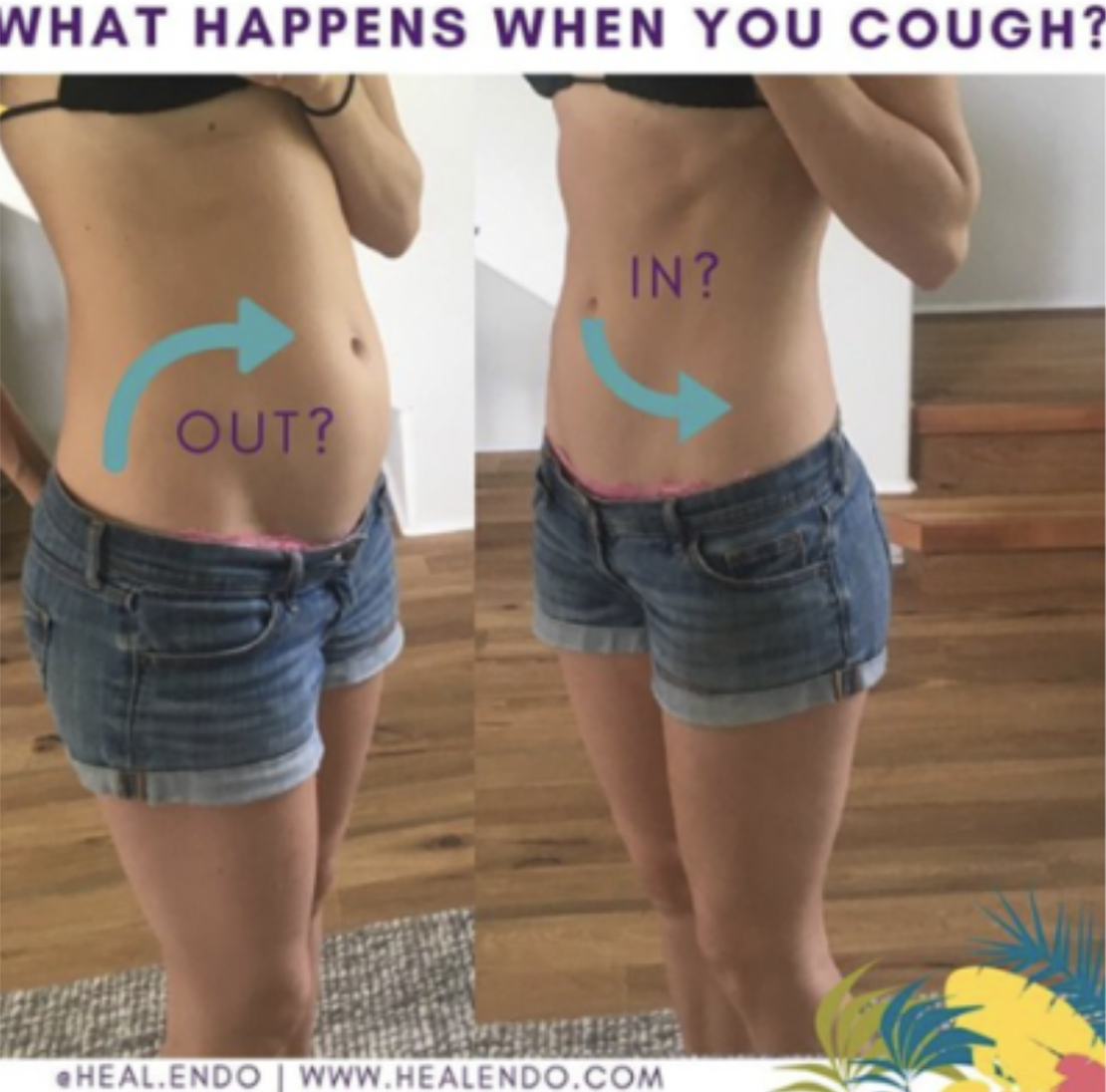
Cough Test: Put one hand on your lower tummy, below the naval, to see what it does. Now, take a breath in and …. cough! Did you feel your lower stomach slightly suck in or brace (yes!), or did it poof out (uh-oh)? If it poofed, it shows your deep core isn’t correctly activating when IAP increases (i.e. core dysfunction).
Rib Test: Look in the mirror while you inhale deeply. Notice if your ribs relax and open wide side to side (yes!), or do they not budge at all and the only way you can take a “deep” breath is if you allow your lower belly to balloon out (uh-oh)? Meet: core dysfunction! Your ribs should not be locked in a static position… ever. They are the key to reducing mismanaged IAP.
Uterus Test: Do you often queef or feel air bubbles come out of your vagina? Do you sneeze pee or leak urine when you run or jump? Does your tampon fall out? Or maybe you can’t insert it all the way because your uterus is that close to your vaginal opening? These are all signs of pressure pushing your organs south, signs of poorly managed IAP and core muscle dysfunction.
Loaf Test: If you lie on your back and do a crunch or double leg lift, do you see a bulge that resembles a “bread loaf” poof out of your tummy? That bulge simply should not be there, as it’s a direct visual of your organs bulging out and down rather than being supported by correctly functioning core musculature.
WHAT TO DO ABOUT CORE DYSFUNCTION?
In my book, Heal Endo, I detail the 5 steps to begin rehabbing the core. There’s a whole chapter in there, actually, because most of us have a deep core system that needs retraining — not harder workouts, but better coordination between breathing, the diaphragm, the transverse abdominis, and the pelvic floor. Restoring this coordination can help redistribute pressure inside the abdominal cavity, support the organs more effectively, and gradually reduce the mechanical forces that contribute to endo belly.
In other words, the goal isn’t simply to strengthen the stomach — it’s to restore the natural pressure system of the body, so that movement once again feels supported rather than strained.
For the sake of this blog post I’m going to talk about 3 factors to start
STRENGTHEN THE RIBS: THE SECRET TO REDUCING ENDOMETRIOSIS BELLY
Remember a moment ago when I asked you to look in the mirror while you inhaled to see if your ribs budged? You may not have been able to do this because you’ve been “breathing” in the wrong place: the tummy.
“But I thought deep belly breathing was good?” you ask.
Deep belly breathing is great—when lying down. It’s done by totally relaxing your abdominal and pelvic floor muscles, and inhaling deeply. As your diaphragm descends down, it pushes on your organs down as well, which is why you see your lower belly rise. This relaxes your deep core and pelvic floor while reminding your body how to let your diaphragm descend (many of our diaphragms are so weak they need help like this to wake up).
But when you’re up and moving and grooving, most of your breath (and the increased pressure that comes with it) should stay in your thoracic cavity, not down on your uterus.
To begin rehabbing, you need to strengthen the terribly atrophied rib muscles (called the intercostals) as well as train the diaphragm to expand side to side rather than drop down (didn’t know your diaphragm was supposed to be strong and expand wide? Now you do!). You will also need to retrain the breathing pattern you’ve been nursing for perhaps decades–shallow chest breathing. Here are some tips:
Back Breathing: Inhaling through the nose, force the air in through the back (visualize an imaginary spot on your back, just below your navel). Imagine the muscles in between the ribs relaxing and expanding the entire back and sides of the ribcage as if it’s growing twice the size. As you do this, you should also be able to visually see the front of your ribcage spread open from side to side.
If your shoulders are tense while you do this, or you shrug your shoulders as you breathe (often a sign of a shallow breathing pattern), take them out of the equation while you wake up the breathing musculature. Lie on your back with your arms relaxing on the bed above your head; now try.
Still having trouble not breathing shallowly in the upper chest? If so, place one hand on your chest for awareness, and now try to force the inhalation lower into the “back” while making sure your hand doesn’t move. It doesn’t matter if you’re belly breathing while you do this (as long as you’re lying down), just stick with this exercise until your ribs can move more easily, and your diaphragm can widen from within. It could honestly take a few weeks if your breathing musculature is severely compromised.
Taking deep breaths and practicing relaxation techniques can help manage pain and stress during endo belly flare-ups. Gentle movement and heat can also help ease tension and keep your bowels moving, which may provide additional relief.
Whereas before your ribs were locked and your breathing pattern confined to your upper chest and lower belly, you’re now on your way to having your ribs and diaphragm to do the breathing work for you as they should!
TEXT BOX: How making more rib space reduces belly bulge
Here’s a perfect example using me 6 weeks postpartum. In the pic on the left, I locked my ribs closed the way they used to be, shrinking room for the diaphragm. As space shrunk, my tummy had to give and - POP- there they are, organs popping right out go my lower belly! This used to be me all the time, and why I always “sucked in”. Instead, to correct on the right, I relaxed my ribs and imagined growing taller in posture. This naturally activates the deep core WITHOUT sucking in, and voila: organs lifted back up. Pretty cool huh? It can take a while to get here where the core naturally activates like that, but it will happen with training, and without you even thinking about it.
2) ADD SOME DEEP CORE TO REALLY POP THE BLOATED BELLY
Once your ribs can move again (thanks goodness), add this next step:
Standing tall (like an invisible rope is lengthening you towards the ceiling), inhale gently through the ribs. As they open wide, keep them open as you gently exhale— use the rib strength to keep the ribs wide! This means your tummy will need to the strong as you exhale in order to keep your ribs as wide as they can go.
Repeat this pattern as long as you can, inhaling and exhaling while trying hard to keep as much room as possible in the thoracic cavity. This will start to remind your deep core to use it’s own strength (rather than tension) to hold your upper body up. If your core is very weak, you may shake a little bit.
Retaining your ribcage to have strength like this will help to widen it, and relax it, which is key for the lower belly bulge to disappear.
3) REDUCE BLOATING WITH PELVIC FLOOR SUPPORT
Here is where I recommend for the millionth time to get thee to a pelvic floor physical therapist! They can help you understand how your pelvic floor is behaving (or misbehaving) and provide specific manipulation, breathing, and activation techniques to rehab this lovely group of deep core muscles.
Additionally, techniques such as gentle abdominal massage can be really helpful.
4) Invest in PROGRAMS:
If you can swing it, I love this program taught by Dr. Angie, the core guru who retrains cores to function optimally! For example, if you failed the cough test, you will pass it after this program. You can also check these videos she made for you, right here. In addition, Move Like a Mutha is often suggested as a helpful core rehab program.
ENDO BELLY FEEL AND EMOTIONAL IMPACT
Look, living with endo belly isn’t just about dealing with a bloated abdomen or severe abdominal bloating—it’s also about navigating the emotional rollercoaster that comes with it. For many, the physical sensation of endo belly is unmistakable: a tight, hard, and often painful swelling in the lower abdominal region that can make you feel like you’ve swallowed a balloon. This isn’t your typical bloating after a big meal; endo belly symptoms can be so severe that they disrupt your daily routine, making even simple tasks feel overwhelming.
But the impact doesn’t stop at physical discomfort. The visible abdominal bloating and pelvic pain can take a real toll on self-esteem and body image. It’s not uncommon to feel embarrassed or self-conscious about your appearance, especially when your clothes suddenly don’t fit or you look several months pregnant—sometimes in just a few hours. This can lead to anxiety, depression, and even social isolation, as you might find yourself avoiding gatherings or activities out of fear of discomfort or unwanted attention.
Relationships can also feel the strain. The combination of severe bloating, digestive discomfort, and pelvic pain can make intimacy challenging, and the emotional weight of managing endo belly can affect communication with loved ones. It’s important to remember that these feelings are valid, and you’re not alone in experiencing them.
That's why I'm here to lovingly remind you that addressing endo belly requires a holistic approach that addresses both the body and mind. Examples include:
Avoiding trigger foods like gluten, dairy, and processed sugars can help reduce endo belly symptoms.
Gentle exercise, like yoga or walking, supports gut health and helps manage stress, both of which are crucial for reducing endo belly flare-ups. Regular exercise can reduce pain caused by endo belly over time by improving blood flow and reducing stress.
Practicing deep belly breathing, meditation, or other relaxation techniques can also help calm the nervous system and reduce anxiety related to endo belly.
Heat therapy using a heating pad can relax muscles and alleviate cramping associated with endo belly. Heat helps muscle tissue to relax, which soothes cramps.
Of course, don’t hesitate to seek support from healthcare providers, therapists, or support groups who understand the challenges of endometriosis and endo belly! Sometimes just talking to someone who “gets it” can make a world of difference.
Ultimately, managing endo belly is about more than just reducing physical symptoms—it’s about caring for your emotional well-being, too. By addressing both sides of the equation, you can take meaningful steps toward feeling better, inside and out.