The Ultimate Guide to Endometriosis Self-Care: Reclaiming Your Life Beyond the Flare
When we talk about endometriosis self-care, the conversation often defaults to bubble baths and dark chocolate. But for those of us living with endometriosis symptoms, self-care isn't a luxury—it’s a biological necessity. It is the active process of calming an overactive immune system, reducing endometriosis inflammation, and mending the pelvic tissues that have been under siege.
I know this journey because I lived it. I went from being a "vegetarian crusader," obsessed with health trends yet stuck in a cycle of infertility, fatigue, and chronic pain--to finding full clinical remission by changing how I cared for my body's stress response system: everything from nutrition and movement to nervous system regulation and chemical exposure reduction.
I was so passionate about understanding the process about it, I wrote a best-selling book titled Heal Endo: An Anti-Inflammatory Approach to Healing From Endometriosis.
Over the years, I have received so many emails regarding "self-care" though. While this is a pretty new-age term, meaning different things to different people, the foundations of the term are essential when healing from any chronic illness. Namely: you need to take care of yourself in order to heal from the longter term conditions. Moreover, with the goal of remission, you need to maintain self care throughout your years in order to keep symptoms at bay.
While my book is the ultimate guide to understanding what endometriosis is, and what true self-care looks like (the kind that aims to help get you into remission), this short, internet-friendly guide is your roadmap to doing the same.
P.S. Make sure to click all the links that take you to other blog posts to better understand why this specific way of "taking care of oneself" is so beneficial for those of us with endo! This post itself is a bit short and summarized, but only because I've already written quite in depth about this information elsewhere.
Understanding Endometriosis Symptoms and the Need for Change
As I'm sure you know, endometriosis involves more than just "bad periods." It is a systemic, inflammatory disease where endometrial-like tissue grows outside the uterus, often on pelvic organs like the bladder, bowels, or ovaries. These endometriosis lesions respond to inflammation, immune factors, chemicals, minerals/nutrients, hormonal changes, stress, the menstrual cycle, and many more things (why endometriosis is known as a multi-factorial disease). This "inflammatory soup" of issues can lead to super fun symptoms like infertility, pain, internal bleeding, scar tissue, fatigue, and more.
If you want to see a variety of other endo symptoms you may never had neard of, check this out.
Why Self-Care is Actually More About Symptom Management
Symptom management for endo isn't about "curing" lesions, but the real reason why is just as important. Let me explain.
First, you can have very small lesions that cause intense pain or other symptoms. In this scenario, your symptoms are worse than the lesions, so self-care to reduce the symptoms is critical. Your quality of life is just as important (or more important in many ways) than what your lesions are doing. Do give a specific example, although I had endometriosis lesions I was dealing with infertility. After a radical self-care campaign, I was able to get pregnant. S
Two, by reducing your stress/anxiety/worry, reversing nutrient deficiencies and balancing blood sugar, improving pelvic circulation (etc etc etc), you can actually change the environment in which those lesions live. This may mean that, by focusing on some real self-care (not the bubble baths and chocolate I mentioned, although those are nice too), you may be able to influence how the disease behaves.
Because, if you didn't know, endometriosis can stabilize or regress, and, according to many studies I list here, it may actually be more likely than progression. (I'm seroiusly not making it up, read the research). So, by focusing on lovely self care factors like hormonal balance and nervous and immune system regulation, we can reduce symptom severity and drastically improve your quality of life.
Self Care and The Impact of Chronic Stress on Endometriosis
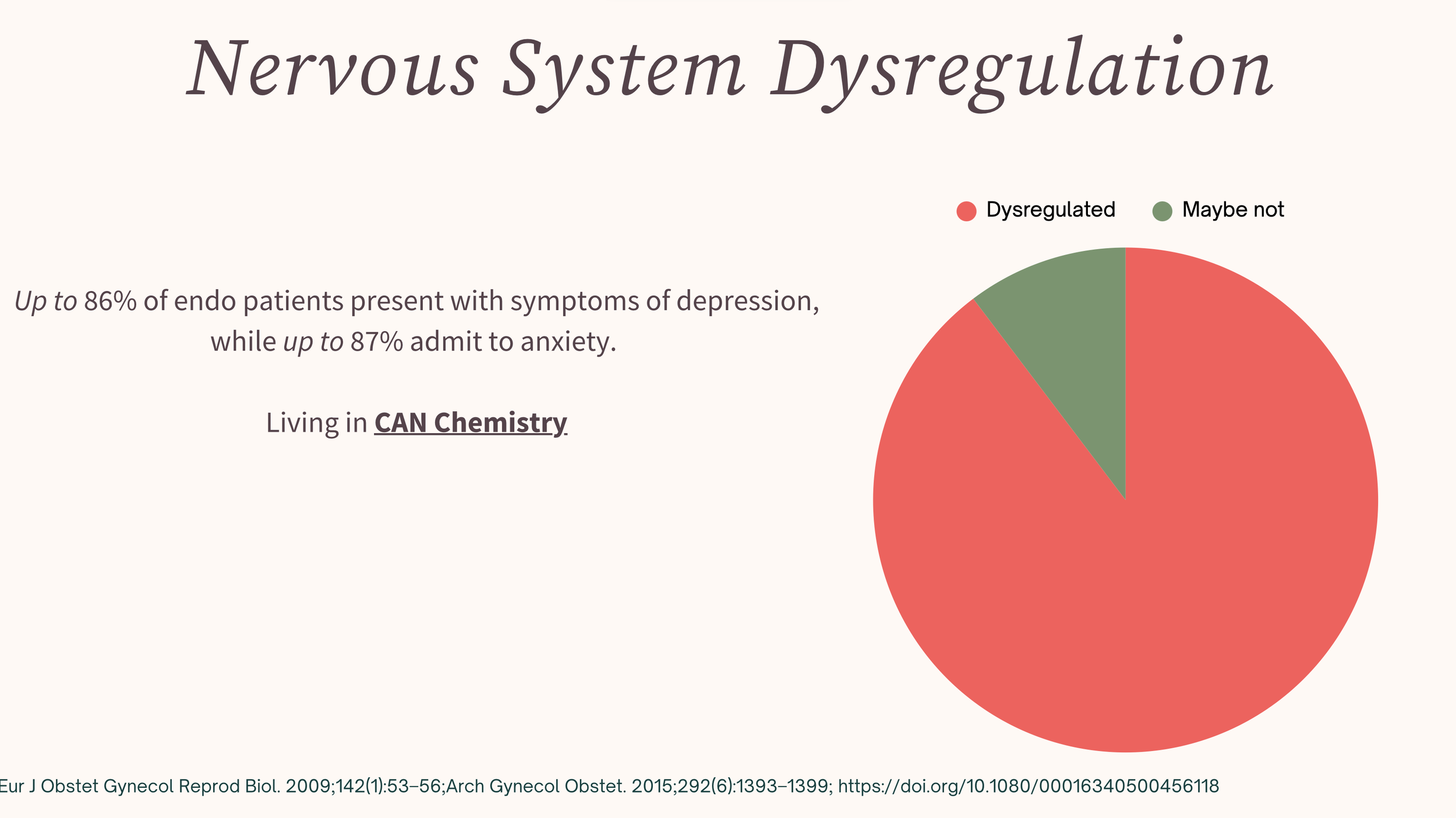
If there is one "secret" trigger for endometriosis flare ups, it is chronic stress. People with endometriosis report higher levels of stress than those without the condition, with 68% experiencing mild to high stress levels. It's why I have numerous chapters about this in my book.
As you can see, most of us with endometriosis are living with nervous system dysfunction, probably without realizing it.
How Stress Worsens Endometriosis Inflammation
Ongoing stress acts as fuel for the fire. Chronic stress can worsen the inflammatory response associated with endometriosis by disrupting the body's stress-response system and altering stress hormones like cortisol and adrenaline.I have a whole article here on how stress makes endometriosis worse, both symptoms and lesions.
The Role of Stress Hormones: Cortisol and Adrenaline
When you are under physical stress or emotional distress, your body floods with stress hormones. These hormones can exacerbate endometriosis symptoms by increasing inflammation and pain sensitivity. Furthermore, stress can trigger the development and growth of endometriosis lesions, as shown in animal studies.
Managing Stress to Break the Cycle
The relationship between stress and endometriosis is cyclical: stress worsens symptoms, and those symptoms increase stress levels. Breaking this cycle through stress management techniques and nervous system regulation is vital to managing endometriosis long-term.
Self Care and the Importance of Managing Endometriosis Flare-Ups
An endometriosis flare-up is a sudden and often severe worsening of symptoms. Understanding what causes an endometriosis flare is the first step in learning to manage pain effectively. I know many women who, after many trials and error, know exactly what their body needs to avoid flare ups, or how to mitigate them when they arrive.
What Triggers an Endometriosis Flare?
Flare ups can be triggered by various factors, and luckily they can also be mitigated pretty well by proper self care considerations: including
Eating well: To help with flares associated with hormonal imbalances, the menstrual cycle, or to avoid foods that provoke inflammation in you (because we're all different, these foods may be fine in some but provoke symptoms in others: High FODMAP foods, dairy, gluten, eggs, or processed foods).
Addressing Stress: To help with jigh ongoing stress levels and nervous system dysfunction.
Factoring in Movement: to adddress pain associated with sex or deep penetration, pelvic floor dysfunction, or posture.
Addressing Environmental risk factors: like alchohol, chemicals, allergens, mold, etc.
The 4 Pillars of Endometriosis Self-Care
To make things easy, throughout my work at Heal Endo, I outline a 5-pillar framework for managing symptoms: Nourish, Reconnect, Mend, Move, and Detox.
Pillar 1: Nourish with an Anti-Inflammatory Diet
What you put on your plate directly impacts systemic inflammation, immune signalling, nervous system regulation, and estrogen processing. So eating an anti-inflammatory diet that focuses on nutrient density rather than deprivation is essential.
Incorporating Anti-Inflammatory Foods
A balanced diet rich in anti-inflammatory foods can help manage inflammation and reduce the severity of endometriosis symptoms. Focus on:
Omega-3 fatty acids (found in cold-water fatty fish) to reduce inflammatory markers.
Antioxidant-rich foods like deep purple berries and leafy greens.
High-fiber foods to help the body eliminate excess estrogen.
Quality Protein: to help balance blood sugar, maintain muscle and repair tissues damaged from inflammation.
Foods to Limit or Avoid
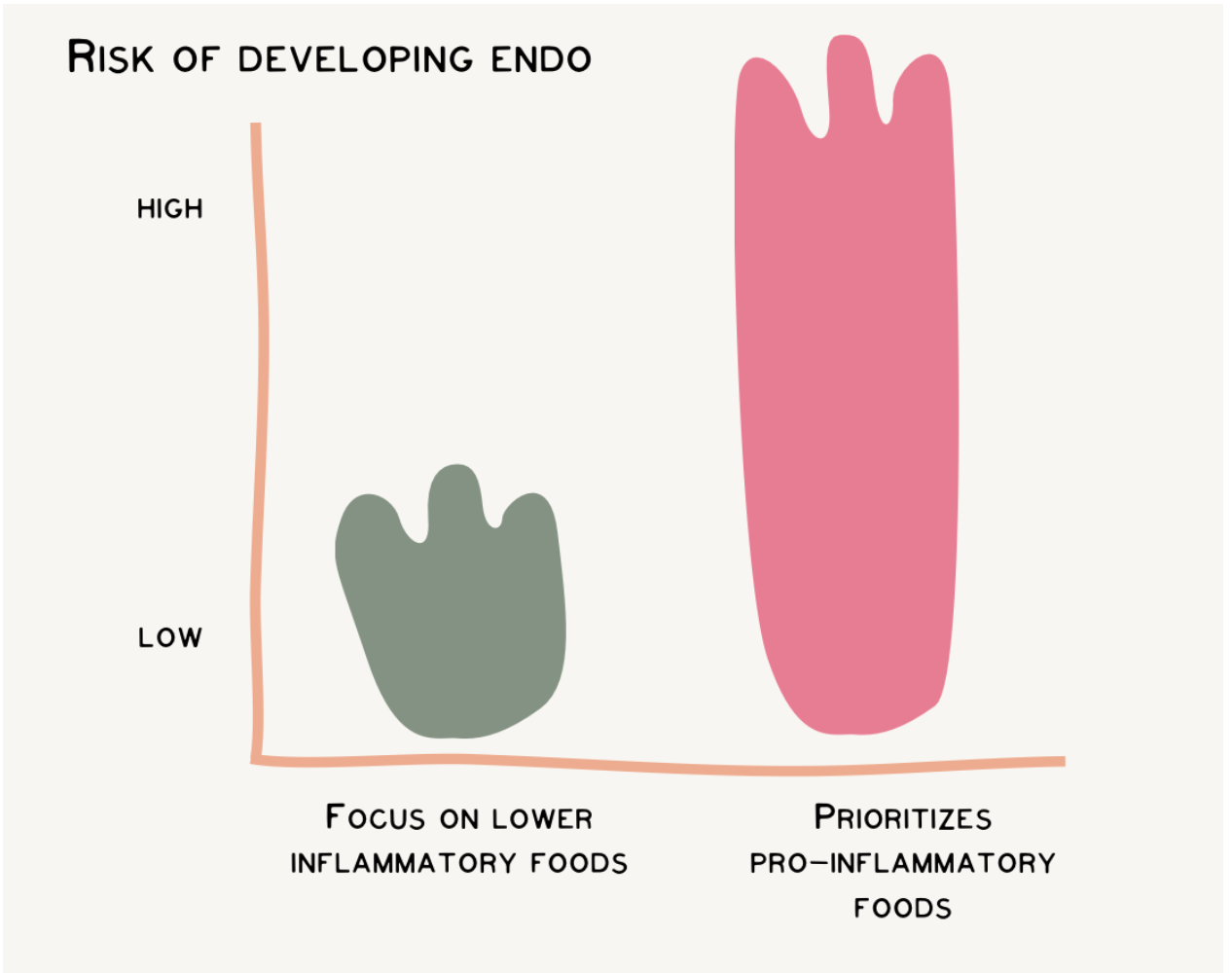
Avoiding inflammatory foods can help prevent unnecessary increases in inflammatory markers. I have a great article here that explains the science behind this, and how pro-inflammatory foods are associated with a greater risk of developing endo. This includes minimizing:
Processed foods and refined sugars.
Alcohol and excess caffeine consumption.
Gluten and conventional dairy products if they are personal triggers.
Diet, Hormonal Balance, and Estrogen Metabolism
Endometriosis is often called an "estrogen-dependent" disease. Achieving hormonal balance is key to preventing the growth of lesions.
The Role of Fiber and Phytoestrogens
A diet rich in fiber can help the body process and eliminate excess estrogen, reducing the hormonal stimulation of endometrial cells.
Maintaining Stable Blood Sugar
Maintaining stable blood sugar levels can prevent insulin spikes that may increase estrogen production and contribute to the development of endometriosis lesions. Moreover, blood sugar imbalances are associated with many factors that go into endometriosis issues.
Pillar 2: Reconnect through Stress Reduction Techniques
Managing stress isn't just about "relaxing"; it's about retuning your nervous system. In fact, if you have nervous system dysfunction, you may not be able to feel like you can relax at all. Instead, try these self care options that help recalibrate the nervous system response.
Pottering: The Lost Art of Pacing for Endo
The difference between “pottering” through chores or rushing through with urgency can be a sink or swim moment for those with chronic illness
When we talk about movement, we often jump straight to "exercise." But for the endo body, high-intensity workouts can often trigger a body's stress response system that leaves us bedbound. This is where the art of Pottering comes in—it is my secret weapon for endometriosis self-care.
What is Pottering?
Pottering is the opposite of a "workout". It is gentle, non-linear movement throughout the day. It’s the act of being upright and moving without a destination or an elevated heart rate. In Britain, to potter is a verb that means to move around in a relaxed way, doing small jobs without any particular plan or urgency. The present participle — pottering — describes that gentle rhythm of movement: the act of simply being involved in ordinary life, in no hurry at all.
The word itself is so pleasant — so perfectly British — and yet its wisdom is profound. Pottering is about moving at your own pace, letting the body catch up with the mind, and remembering that rest can be found in motion when the motion is gentle. It is not about doing less or being lazy! Rather, it’s about doing what you need to do, in a relaxed rhythym rather than a psychotic pace (as I used to move).
Why Pottering Prevents Pelvic Hypoxia
Sitting for long periods is a major trigger for endometriosis pain because it creates pelvic ischemia—a lack of oxygen to the pelvic region. When we sit, we "plug" the blood flow to the pelvic organs. Pottering—spending 10 minutes folding laundry, then 5 minutes watering a plant, then a short stroll to the mailbox—keeps the blood moving through the pelvic cavity without stressing the immune system.
Pacing to Avoid the "Crash and Burn"
For endometriosis patients, pacing is everything. If you have a "good day" and try to do all the chores you missed, you often trigger a massive endometriosis flare-up the next day. Pottering allows you to stay active while maintaining hormonal balance and keeping stress hormones low. Make sure to read my full article on it here.
Mindfulness and Meditation
Mindfulness and meditation techniques can help reduce stress and anxiety associated with chronic pain. I have heard from sooooo many women that, by simply becoming more mindfull in their days, they literally changed the intensity of their symptoms. How cool is that? That’s why I recommend a great self-care focus on these practices, which can lead to a noticeable reduction in pain intensity.
Relaxation Techniques for Pain Perception
Relaxation techniques, such as deep breathing exercises, can help manage the body's stress response system. By lowering your pain sensitivity, you change how your brain interprets pelvic pain!
Neural Rewiring: My personal favorite
A few years ago, I realized that, for all my work on stress, I was still living in a world of nervous system dysregulation. I finally addressed it (and omg did I feel better!) with an online program called DNRS. It's very simple; it just takes time each day to practice, but I think most of us with endo would benefit greatly from it.
Pillar 3: Mend with Gentle Movement
Many endometriosis patients are afraid to move, but regular exercise is one of the best ways to reduce inflammationand improve pelvic tissue health! I write a lot about this in my book, too, but here are some starting pointers.
Heat Therapy, Circulation, and Pelvic Floor Physio
Heat therapy includes applying heating pads or hot water bottles to the pelvic area to relax muscles and ease cramping. This is a great start to help increase blood flow to pelvic tissues, preventing pelvic ischemia (low oxygen). I also can't recommend enough pelvic floor physical therapy; your life will be changed.
The Power of Gentle Exercise
Gentle exercise such as walking, swimming, or yoga can improve circulation to the pelvic cavity and release natural pain-relieving endorphins. This helps "unplug" the pelvic organs and reduce pelvic discomfort. Check out all my articles on movement and posture for a deep dive.
Pillar 4: Detox by Reducing Your Toxic Burden
Why reducing the toxic burden becomes a helpful self-care focus
Our modern world is full of risk factors like endocrine disruptors. Reducing your toxic burden involves making lifestyle choices that support your liver and immune system.
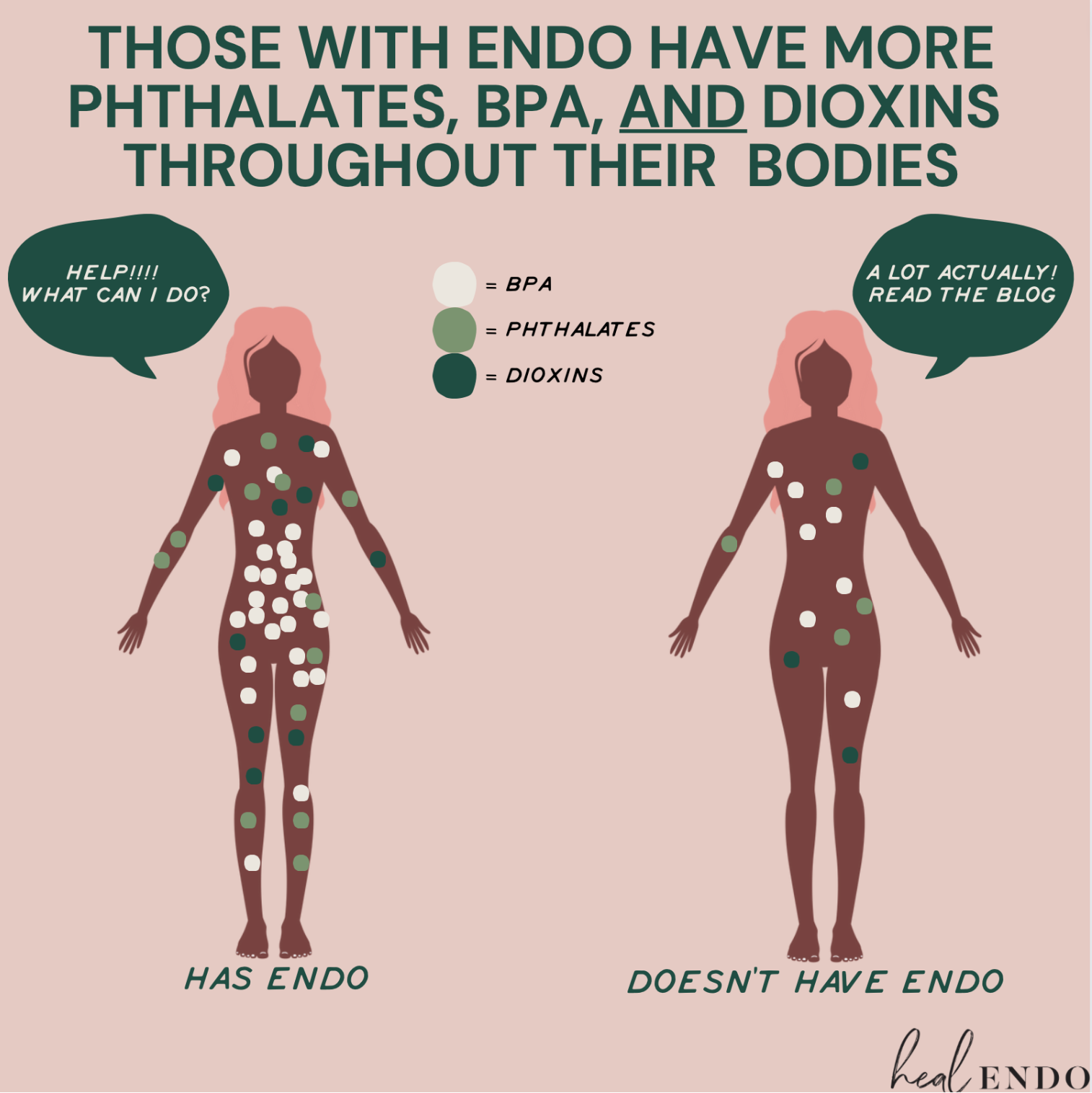
Identifying and Avoiding Some Bigger Endo Triggers: Phalates, Herbicides, Dioxins, Oh my!
As I detail in my book and in this blog, environmental toxins can exacerbate endometriosis in a myriad of ways, from contributing to the creation of an endo-like cell to fostering some of the immune dysfunction associated with the disease. Choosing organic produce and 100% grass-fed meat can help minimize exposure.
Practical Self-Care Tools for Daily Life
Beyond the big pillars, small lifestyle choices impact the frequency and severity of symptoms.
Prioritizing Sleep Hygiene
Prioritizing good sleep hygiene helps the body recover from chronic pain and manage fatigue. Quality sleep is vital for supporting immune function and hormonal equilibrium. This sounds so easy it's boring. HOWEVER (sorry to yell), but many of us forego the conditions that help with sleep in order to get more screen time in: Netflix, scrolling, movies, you name it.
Staying Hydrated
Staying well-hydrated helps support overall health and can alleviate some symptoms, such as painful bowel movements or pelvic inflammatory disease sensations. Another easy win!
Maintaining a Symptom Diary
Maintaining a symptom diary can aid in tracking pain severity, menstrual cycles, and dietary triggers. This helps you identify personal triggers so you can take timely action. Moreover, it can make you feel more stable when understanding when and why you have symptoms.
The Role of Professional Support
Of course, endometriosis self-care can be more effective when supported by healthcare professionals.
Physical Therapy for Pelvic Pain
Again, physical therapy, specifically pelvic floor PT, can be life-changing for manage pain and addressing scar tissue.
Mental Health and Support Groups
Psychological support is important for individuals with endometriosis. Connecting with support groups can help in coping with the mental burden and emotional distress of the disease.
Navigating Hormonal Treatments and Surgery
While birth control pills and hormonal treatments can suppress symptoms, they don't always address the root cause. Working with a specialist helps you make informed decisions about managing endometriosis. This goes for surgery too! For a list of vetted specialists, I recommend icarebetter.com
Your Endo, Your Rules: Reclaiming the Narrative
If there is one thing I want you to take away from this guide, it’s this: You are not a passive bystander in your own body. For too long, the narrative around endometriosis has been one of "grin and bear it," or worse, "here’s a prescription and a surgical date—see you in six months." But as we’ve explored, your body isn't "broken"; it’s overwhelmed. It’s reacting to a world of inflammatory triggers, oxygen-starved tissues, and a nervous system that thinks a leopard is perpetually chasing it.
Self-care isn't about being perfect! It isn't about never eating a cupcake again or spending four hours a day in a meditative trance. It’s about Pottering instead of pushing. It’s about choosing a juicy ribeye because your cells are screaming for zinc. It’s about finally giving your pelvic organs the "breath of fresh air" they’ve been waiting for by going to pelvic floor PT.
Want the Full Map? Let’s Dive Deeper.
If you’re ready to stop guessing and start healing, my book, Heal Endo: An Anti-Inflammatory Guide to Healing from Endometriosis, is your deep-dive companion. Think of it as the ultimate "User Manual" for your body that your doctor never gave you. Inside, we go way beyond the basics, breaking down the 4 Pillars with over 400 clinical citations and a whole lot of heart.
Whether you are just starting to track your symptoms or you’re a seasoned "endo warrior" looking for that missing piece of the puzzle, remember: Remission isn't a myth, and you are worth the effort it takes to get there.
So, put down the "hustle," pick up a watering can (it’s time for some Pottering!), and let’s start mending. You’ve got this, and I’m right here with you.
Scientific References & Further Reading
On Stress & Inflammation:
Guo, S. W., et al. (2017). Social psychogenic stress promotes the development of endometriosis. This research highlights how chronic stress doesn't just feel bad—it can actually accelerate the progression and development of endometriosis lesions by altering the immune response.
Long, Q., et al. (2016). Chronic stress accelerates the development of endometriosis through adrenergic receptor β2. This study illustrates the physiological link between stress hormones (like adrenaline) and the worsening of the disease.
Brasil, D. L., et al. (2020). Psychological stress levels in women with endometriosis: a systematic review. This meta-analysis confirmed that women with endo report significantly higher stress levels, which in turn exacerbates systemic inflammation.
On Nutrition & Anti-Inflammatories:
Mier-Cabrera, J., et al. (2009). Vitamins E and C as a highly efficient alternative therapy to relieve chronic pelvic pain. This clinical study found that high-dose antioxidant supplementation led to a significant reduction in chronic everyday pain for 43% of endo patients.
Harris, H. R., et al. (2013). Dairy-food, calcium, magnesium, and vitamin D intake and endometriosis. This prospective cohort study linked higher vitamin D status with a lower risk of developing endometriosis and noted its role in modulating inflammation.
Averstad, A., et al. (2018). Antioxidant intake and oxidative stress in women with endometriosis. This research highlights that endo sufferers often consume fewer antioxidants than their peers, making a high-antioxidant diet a critical intervention for quenching free radicals.
On Pelvic Circulation & Hypoxia:
The Angiogenesis Connection: Research in Scientific Reports (2020) and Life Science Alliance (2021) discusses how endometriosis lesions use hypoxic (low-oxygen) environments to trigger angiogenesis—the growth of new blood vessels—which allows the lesions to survive and progress.
Hypoxia as a Survival Switch: Your guide references the modern understanding that pelvic hypoxia (often caused by lack of movement or mechanical tension) acts as a survival "switch" that prevents the immune system from clearing out ectopic tissue.
Ischemia and Pain Perception: Clinical observations in physical therapy, such as those by Dr. Angie Mueller, emphasize that increasing blood and lymph flow to the peritoneal cavity is essential for delivering nutrients and immune factors required for tissue mending.